Swiss Doctors
Main goals
Swiss Doctors is a non-governmental organization operating in different low resource countries. One of the projects is at the Community Hospital in Serabu, Sierra Leone. The main focus of this project is improving mother and child health including newborn care by teaching and training the local health care workers.
Brief description of the project
Sierra Leone is a small country in West Africa facing tremendous maternal and neonatal mortality rates, some of the highest worldwide. The number of doctors for a population of roughly 7 million people is extremely low (156 doctors, WHO Sierra Leone Annual report 2017). The main work in the health care system is therefore done by nurses and community health officers.
In Sierra Leone, the neonatal mortality is 35 out of 1000 live births (WHO annual report Sierra Leone 2017). In this context, it is interesting to note that it is common practise to not give a name in the first weeks to months; the newborns are just called bobor (boy) or baby (girl).
The Serabu Community Hospital is located in a remote area in Sierra Leone and has a long history. It was built in 1954, destroyed during the civil war in the nineties and reconstructed in 2009. Since 2010 our partner organization German Doctors supports the hospital, mainly by sending European doctors continuously for short term placements over the year; since 2018 in collaboration with the newly founded Swiss Doctors NGO.
During the first years, the pediatric focus was set on the two major health problems in Sierra Leone: malaria and malnutrition. In 2014 the neonatal unit with a calculated number 5 beds (maximum capacity up to 12 newborns) was finally built. Unfortunately, there was no further development during the Ebola epidemic for the following 18 months. Since then, great efforts have been made to further develop the neonatal unit and to improve skills and knowledge of the local health care staff.
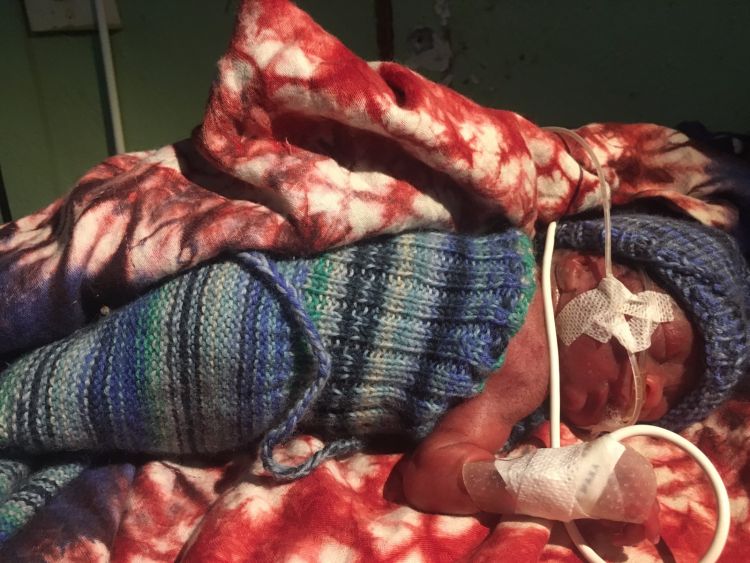
Similar to other low resource countries and corresponding to the data of WHO, the 3 most common neonatal disorders are prematurity, birth asphyxia and infections. In order to improve morbidity and mortality several measures have been implemented: improvement of the quality of regular antenatal care, provision of a new waiting house for mothers with high risk pregnancies and regular teaching of the health care staff (nurses and community health officers) in newborn resuscitation and basics of newborn care such as hygiene, early breastfeeding, temperature control, kangaroo care, blood sugar monitoring, nasogastric feeding, etc.
At this stage, there is only little advanced medical equipment consisting of oxygen saturation monitors and oxygen concentrators as well as medication such as oral coffeine citrate and i.v. antibiotics. Introduction of a CPAP system is planned for the coming year together with a new building for the newborn unit.
Following the successful management of some small preterm babies with birth weights of less than 1000 g, the helath care staff and parents are motivated to support our interventions. There is still of lot of room for improvement. Continuous teaching of the local health workers is necessary in order to get to a point were foreign support is not needed any longer.
Contact information
Swiss Doctors
Postfach
8000 Zürich
Financial support
Donations.
Website


